- Commissioner’s Office
- Community Behavioral Health
- Planning Innovation
- Behavioral Health Division
- 988 Suicide and Crisis Lifeline
- Single County Authority
- Management Services Department
- Contracts & Budgeting
- Behavioral Health Crisis Intervention Services
- Coordinated Consumer Services
- Housing and Homeless Services
- Heat Safety
- Southeast Regional Planning and Implementation
- Crisis Intervention Team Training
- Intellectual disAbility Services
- Administration, Finance, and Quality
- Behavioral Health and Justice Division
Home » About Us » DBHIDS Organization » Division of Administration, Finance, and Quality » Quality Management and Compliance » Compliance Program
DBHIDS Compliance Program
The purpose of the DBHIDS Compliance Program is to ensure providers, programs, operations, and services maintain the highest ethical standards, comply with all local, state and federal laws and regulations, and demonstrate financial responsibility in the delivery of contracted services.
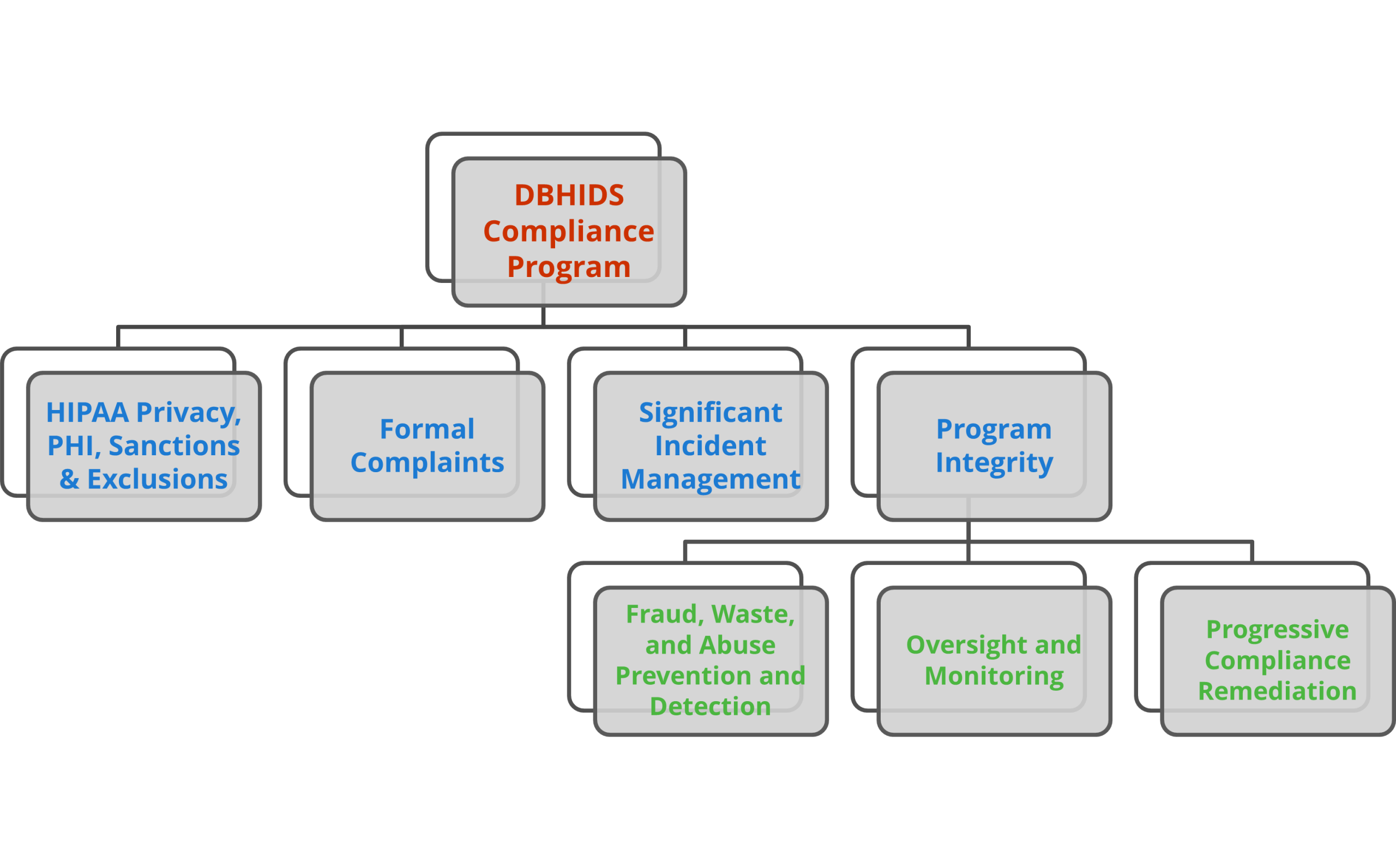
The compliance team is responsible for carrying out the following functions:
HIPAA Privacy and Protected Health Information
The City of Philadelphia complies with Health Insurance Privacy and Accountability Act (HIPAA) by designating specific departments like DBHIDS as “Covered Units.” As a Covered Unit, DBHIDS follows the City of Philadelphia Confidentiality Policies and Procedures and is responsible for protecting sensitive health information, overseeing compliance with privacy rules, sharing the HIPAA Notice of Privacy Practices, and responding to requests for information. This helps ensure that health information is kept confidential and handled securely.
Protected Health Information (PHI) is health information subject to protection under HIPAA. As a covered unit, DBHIDS is responsible for identifying, managing, and maintaining oversight of all PHI under its control and must keep an inventory identifying the types of PHI maintained and the locations in which it is stored. This includes the applicable programs, information systems, and physical locations where PHI is stored.
Disclosure of PHI is strictly regulated. Only the DBHIDS Privacy Officer is authorized to release PHI, and only upon receipt of a valid HIPAA Authorization to Release Personal Health Information Form or a written request that meets the requirements of an individual’s Right of Access under HIPAA. These controls ensure compliance with applicable federal regulations and safeguard individuals’ privacy rights.
Contact DBHIDS HIPAA Privacy
- Telephone 215-685-4763
- Toll-free 888-858-1748
- Fax 215-685-4684
- Email DBHIDS.HIPAA@Phila.gov
- Mail
Attn: DBHIDS HIPAA Privacy Officer
1101 Market St., 7th Floor
Philadelphia, PA 19107
Sanctions and Exclusions
Sanctions and exclusions are enforcement actions administered by the Office of Inspector General (OIG) (mail link) to protect the integrity of federal health care programs. Sanctions may result from administrative hearings or be imposed directly in response to violations of federal or state regulations, civil statutes, or criminal law. Exclusions represent the most severe form of sanction and are typically imposed when an individual or entity is determined to pose an unacceptable risk to the safety of individuals receiving services or to the integrity of health care programs.
To maintain compliance, health care providers and organizations are required to routinely screen employees, contractors, and vendors against applicable federal and state exclusion databases, including the OIG’s List of Excluded Individuals/Entities (LEIE), System for Award Management (SAM), and state Medicaid exclusion lists.
QMaC conducts sanctions and exclusions screenings on a monthly basis to ensure ongoing compliance. Failure to adhere to these requirements may result in significant administrative, civil, or financial penalties, depending on the nature and severity of the violation.
Formal Complaints
Formal complaints are disputes or objections regarding the coverage, operations, or management of behavioral health providers or programs contracted with DBHIDS or concerning DBHIDS employees and DBHIDS practices.
The Formal Complaint process, as outlined in the DBHIDS Formal Complaint Policy ensures that all recipients of DBHIDS services are treated fairly and that contracted providers and programs remain responsive to participants’ needs, particularly with respect to the identification, review, and resolution of complaints. All formal complaints are reviewed, tracked, and monitored by the compliance team.
The Formal Complaint process is structured as a tiered system (Level 1, Level 2, and Level 3) that allows complainants to appeal determinations. Complaints may also be submitted anonymously; however, anonymously submitted complaints do not follow the tiered process.
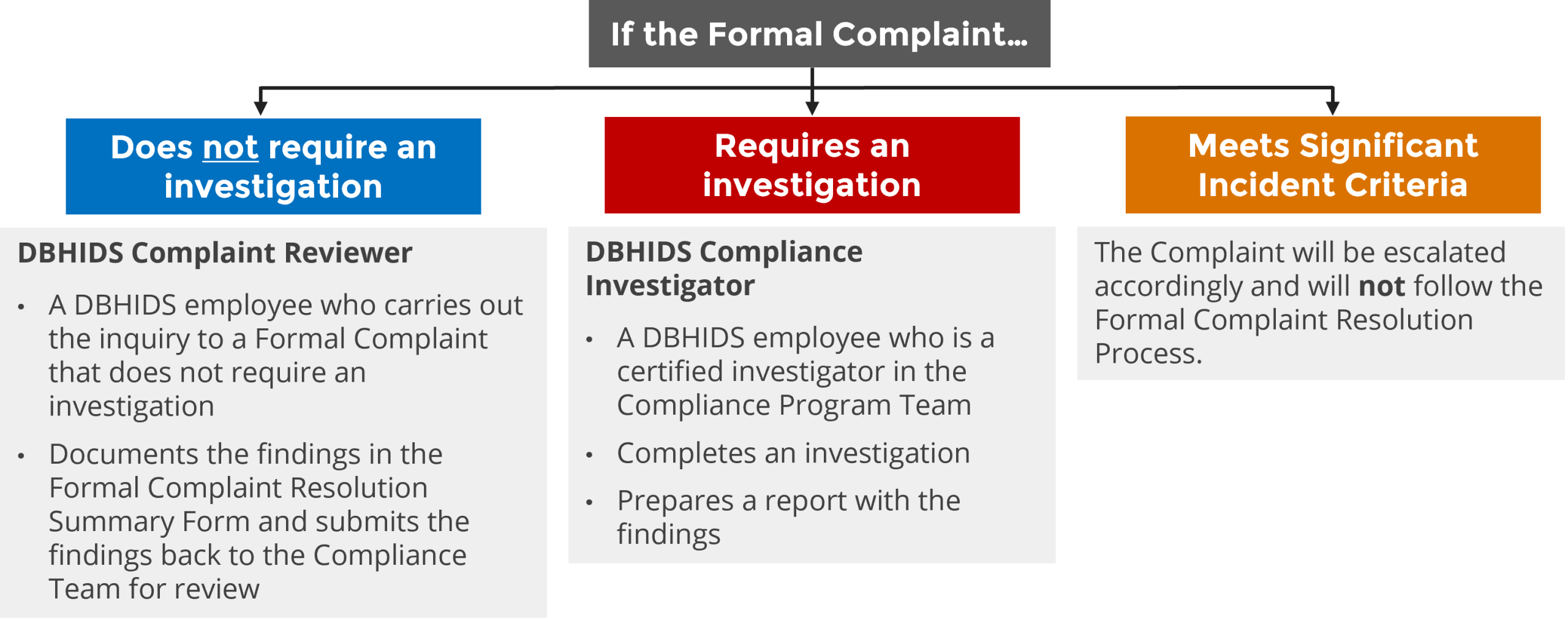
Formal complaints may require an investigation conducted by a certified investigator from the compliance team who then prepare a written report documenting findings and conclusions.
Formal complaints may also be escalated and reclassified as a significant incident. When a complaint is reclassified as a significant incident, it is managed in accordance with the DBHIDS Significant Incident Policy.
Provider disputes are handled differently from other complaints as they typically involve concerns raised against a DBHIDS service and/or practice.
All formal complaints must be submitted using the DBHIDS Formal Complaint Submission Form.
Individuals filing a complaint can designate a personal representative to represent them during the formal complaint process using the Personal Representative Appointment Form.
Medicaid members seeking to file a complaint must contact the Community Behavioral Health Member Services Department, which is available 24 hours a day, seven days a week at 888-545-2600.
Contact DBHIDS Formal Complaints
- Telephone (215) 685-5458
- Toll-free (888) 686-6332
- Fax (215) 685-5580
- Email DBHIDS.Complaints@Phila.gov
- Mail Attn: DBHIDS Formal Complaints; 1101 Market St., 7th Floor, Philadelphia, PA 19107
Significant Incidents Management
Significant Incidents are non-routine events that are harmful or materially threatening, inconsistent with standards of practice, and may jeopardize the health or well-being of an individual receiving services.
Reportable significant incidents categories include: Death, suicide attempt, homicide, adverse medication reaction and/or medication error, emergency services, abuse, neglect, non-routine injury or illness, overdose reversals, emergency room visits and inpatient admissions, missing person, seclusion or restraint.
The primary objective of the DBHIDS Significant Incident Management Policy (PDF) is to enhance the health, safety, dignity, rights, and well-being of individuals receiving behavioral health services while ensuring compliance with applicable state laws, regulations, and guidance.
The objective of the Significant Incident Management as outlined in the Provider Requirements for Significant Incident Management Policy (PDF) is to promote the reporting of significant incidents in order to strengthen prevention, mitigation, and response efforts and ensure timely response and coordination of significant incidents for all county-funded providers and services contracted with DBHIDS.
The Significant Incident Reporting Process applies to all DBHIDS contracted providers, whether licensed or unlicensed.
All providers are required to report Significant within twenty-four hours using one of the following methods:
- Providers servicing individuals in Community Residential Rehabilitation, Long-Term Structured Residences, and Supportive Living Program/Community Hospital Integration Project Program must submit reports through the Home and Community Services Information System utilizing the Enterprise Incident Management system, as described in the Reportable Incident section of the Office of Mental Health and Substance Abuse Services OMHSAS Bulletin 15-01 (PDF).
- All other providers must submit the DBHIDS Significant Incident Report (SIR) Form. For incidents requiring an investigation, providers must submit the DBHIDS Investigation Report Form within 14 days and submit final findings within 30 days.
QMaC reserves the right to complete Formal Investigations, including investigations initiated in response to provider findings documented in the DBHIDS Investigation Report Form, Formal Complaints, Significant Incidents, and NIAC reviews.
The DBHIDS Significant Incident Policy, Management, and Reporting Process do not apply to Intellectual disAbility Services (IDS) and Early Intervention programs. These programs must comply with their respective responsibilities and procedures under the Office of Developmental Programs (ODP) Bulletin 00-21-02 (PDF) governing intellectual disabilities and autism services.
All Significant Incident Reports must be submitted using the DBHIDS Significant Incident Report (SIR) Form via email, mail, fax, or an online form. For incidents requiring an investigation, providers must also submit a Significant Incident Investigation Report.
Contact DBHIDS Significant Incident Management
- Telephone: (215) 253-4315
- Toll-free: (888) 686-6332
- Fax: (215) 685-5564
- Email: DBHIDS.SignificantIncidents@Phila.gov
- Mail:
Attn: DBHIDS Significant Incidents
1101 Market St., 7th Floor
Philadelphia, PA 19107
Program Integrity
DBHIDS is committed to safeguarding resources, promoting accountability, and ensuring that services are delivered ethically, efficiently, and in compliance with federal, state, and local laws and regulations. Efforts of Program Integrity are organized around the following core focus areas:
Fraud Waste and Abuse (FWA) Prevention and Detection
- This focus area ensures that DBHIDS programs, services, and resources are protected from misuse, mismanagement, and intentional wrongdoing. QMaC actively works to identify potential FWA red flags and encourages the referral of suspected concerns to the Compliance Hotline.
- QMaC also conducts random audits to verify that services billed and paid for accurately reflect services provided and are supported by appropriate documentation.
- Fraud is the intentional deception or misrepresentation made with the knowledge that it could result in an unauthorized benefit.
- Waste is the misuse, mismanagement, or overutilization of resources that results in unnecessary cost to the system.
- Abuse refers to actions that are inconsistent with sound fiscal, business, or medical practices, resulting in avoidable costs or improper use of services.
- Examples of Fraud, Waste and Abuse include:
- Extortion: The use of threats, coercion, or intimidation to unlawfully obtain something of value.
- Bribery: Giving something of value to influence someone’s behavior for gain.
- Kickbacks: Illegal payment intended as compensation for preferential treatment.
- Employee misconduct: Behaving with substantial or intentional disregard for the employer’s interest or the company’s code of conduct.
- Misuse of employee property: A substantial or intentional disregard for the employer’s property.
- Theft of time: Misrepresenting work hours by claiming time that was not actually worked.
Progressive Compliance Remediation
- Progressive Compliance Remediation is a structured and collaborative process used to address compliance concerns identified from Formal Complaints, Significant Incidents, confirmed Fraud, Waste, and Abuse, NIAC reviews, and other compliance monitoring activities. This process is also used when evaluating provider performance related to noncompliance with regulatory requirements or the provider agreement.
- When required standards are not met, or when programmatic, operational, fiscal, staffing, training, and/or clinical deficiencies persist, this progressive approach provides an opportunity to correct deficiencies and achieve compliance by utilizing steps to ensure that operations and practices meet established standards through evaluation, resolution, and continuous quality improvement.
- Provider Progressive Compliance Remediation Measures include:
- Verbal notice and provider coaching.
- Provider meeting.
- Corrective Action Plan (CAP).
- Directed Corrective Action Plan (DCAP).
- Closure of admissions.
- Termination of current contract/funding.
- No renewal of contract/funding for the next fiscal year.
- Internal DBHIDS Progressive Compliance Remediation Measures include:
- Action plan.
- Quality Improvement Plan (QIP).
- Corrective Action Plan (CAP).
- Progressive Compliance Remediation Measures are not intended to be punitive but collaborative and corrective, focusing on support and improvement.
- The type and intensity of remediation are determined by the severity, scope, and frequency of the identified issue.
Oversight and Monitoring
- DBHIDS Compliance functions encompass both internal business unit compliance and quality improvement activities.
- Oversight establishes standards, expectations, and governance structures.
- Monitoring evaluates whether those expectations are being met through ongoing review and data validation.
- Internal DBHIDS Oversight and Monitoring include routine reviews of DBHIDS units to promote accountability, transparency, and continuous improvement, including efforts to:
- Ensure policies and procedures are current, compliant, and effectively implemented.
- Identify and address potential issues before violations occur.
- Promote a culture of accountability, transparency, and continuous improvement.
- Monitor the implementation and effectiveness of Progressive Compliance Remediation activities.
- Provider Oversight and Monitoring include compliance activities related to provider and individuals receiving services, which may occur through:
- Formal complaints.
- Significant incident reports.
- NIAC site reviews.
- Findings of noncompliance with contractual and regulatory requirements.
Contact DBHIDS Compliance Program
- Hotline: 215-253-7763
- Toll-free: 888-686-6332
- Fax: 215-685-5565
- Email: DBHIDS.Compliance@Phila.gov
- Mail:
Attn: DBHIDS Compliance Program
1101 Market St., 7th Floor
Philadelphia, PA 19107
 City of Philadelphia
City of Philadelphia

